News and Announcements
Read the latest news from Northwestern University Feinberg School of Medicine’s Department of Ophthalmology. The links below take you to articles where you can learn more about our faculty’s latest achievements, awards and honors.
 03.27.2026
03.27.2026Northwestern Medicine scientists have discovered that light plays a key role in how animals perceive environmental threats, findings that could improve the understanding of risk avoidance behaviors and disorders in humans, according to a recent study published in Nature Communications.
 10.29.2025
10.29.2025A recent study led by Tiffany Schmidt, PhD, has discovered previously unknown cellular mechanisms that shape neuron identity in retinal cells, findings that may improve the understanding of brain circuitry and disease.
 10.06.2025
10.06.2025Patients with newly diagnosed glaucoma who have less wealth or reside in rural communities are less likely to receive standard glaucoma care compared to wealthier patients, according to a recent multi-institution study published in JAMA Ophthalmology.
 01.10.2025
01.10.2025The Department of Ophthalmology has received a grant from Research to Prevent Blindness to support investigators advancing the field of ophthalmology and vision science.
 09.13.2024
09.13.2024Patients who live in rural communities, Hispanic patients and Black patients with pre-existing diabetic retinopathy are less likely to receive annual diabetic eye exams than white patients, according to a recent Northwestern Medicine study.
 09.11.2024
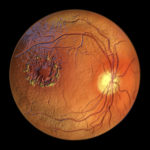
09.11.2024Northwestern Medicine investigators have shed new light on how white blood cells in the retina function during inflammation and possibly during retinal vascular diseases with inflammatory components like diabetic retinopathy, according to a study recently published in the Journal of Clinical Investigation.
 06.10.2024
06.10.2024Northwestern Medicine investigators have identified novel genetic mechanisms that regulate blood vessel growth in the retina and may also serve as therapeutic targets for retinal vascular disease, according to findings published in Nature Communications.
 02.13.2024
02.13.2024An individual retinal cell can output more than one unique signal, according to a Northwestern Medicine study published in Nature Communications, a finding which sheds new light on the complexities of how vision functions in mammals.
 01.09.2024
01.09.2024Northwestern Medicine scientists have identified how a subset of neurons enable the eyes to perceive motion, according to a study published in Nature Communications, a discovery that reveals previously hidden complexities of how vision functions in mammals.
 10.20.2023
10.20.2023Investigators have discovered a new subtype of interneurons in the retina that allows the eye to see and identify objects better in both the light and in the dark, dismantling previous notions about the inner workings of the retina, according to a Northwestern Medicine study.
 06.16.2023
06.16.2023A Northwestern Medicine study has uncovered novel cellular mechanisms within the retina, findings that could help advance the development of targeted therapeutics for diseases and conditions impacting vision.