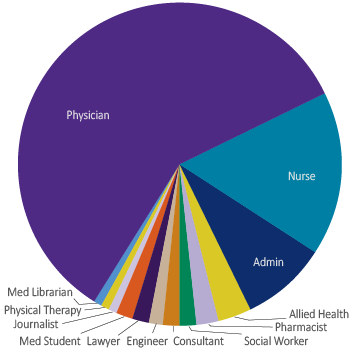
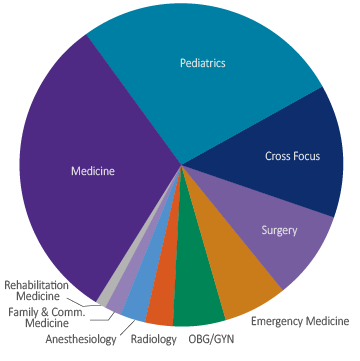
As part of their learning and the program’s evaluation of HQPS content and skill mastery, students design, implement and complete a capstone project that demonstrates students’ leadership capacity and capability to conduct improvement in healthcare. Some students implement improvement projects in their local home institutions, while others seek to have statewide, national and international impact.
Example Capstone Projects
- Development of standardized shoulder dystocia drills for clinical obstetrical staff at NorthShore University Health System. (RN, Illinois)
- Development and implementation of structured inter-disciplinary rounds, which reduced adverse events by 50 percent in intervention units as compared to controls units at Northwestern Memorial Hospital. (MD, Illinois)
- Pertussis immunization improvement project resulting in an 82 percent increase in administration in the ED and a 14 percent increase in the urgent care setting from baseline at Mercy Health System. (PharmD, Wisconsin)
- Developing the infrastructure and responsible board for a combined international reporting system repository for device-related adverse event reporting. (MBA, International)
- Design and implementation of the Healthcare Leadership in Quality curriculum for residents at Penn Medicine. (MD, Pennsylvania)
- Development of a provincial trauma transfer protocol for patients moving from Prince George Regional Hospital to Vancouver General Hospital. (British Columbia, MD)
- First implementation of a program of early childhood developmental screening and follow-up in Mexico, including appropriate metrics, as well as establishing national reimbursement for these services for providers in Mexico. (Instituto de Pediatría, Techológico de Monterrey, MD, Mexico)
- Improved access to care for the inmates in the San Francisco County Jail with a standardized sick call process and triage guidelines and implementing a revised medical care request form to solicit better information from the patients. (MSPH, California)
- Development of an early warning system and subsequent steps to reduce sepsis mortality by 36.6 percent and annual mortality by 20 percent at the University of Illinois Hospital and Health Sciences System at Chicago. (MBA, Illinois)
- Development of a toolkit to reduce workplace violence against healthcare professionals from patients across institutions affiliated with the Washington State Hospital Association. (RN, JD, Washington)