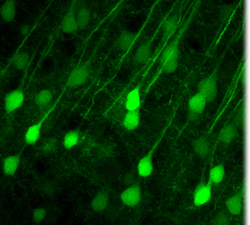
A small group of elusive neurons in the brain’s cortex play a big role in ALS (amyotrophic lateral sclerosis), a swift and fatal neurodegenerative disease that paralyzes its victims. But the neurons have always been difficult to study because there are so few of them and they look so similar to other neurons in the cortex.
In a new preclinical study, a Northwestern Medicine® scientist has isolated the motor neurons in the brain that die in ALS and, for the first time, dressed them in a green fluorescent jacket. Now they’re impossible to miss and easy to study.
The cells slide on neon jackets when they are born and continue to wear them as they age and become sick. As a result, scientists will now be able to track what goes wrong in these cells to cause their deaths and be able to search for effective treatments.
“We have developed the tool to investigate what makes these cells become vulnerable and sick,” said Hande Ozdinler, PhD, senior author of the study and assistant professor of neurology at Northwestern University Feinberg School of Medicine. “This was not possible before.”
Ozdinler and colleagues also identified the motor neurons that don’t die, enabling scientists to study what protects them.
The study was published in The Journal of Neuroscience on May 1.
ALS, also known as Lou Gehrig’s disease, causes the death of muscle-controlling nerve cells in the brain and spinal cord (motor neurons). It results in rapidly progressing paralysis and death usually within three to five years of the onset of symptoms.
There are about 75,000 upper motor neurons affected in ALS out of some 2 billion cells in the brain. Previously, the only way to study the upper motor neurons was to extract them through surgery, a difficult process that was beyond the scope of most scientists and still didn’t allow examination of the ailing neurons at various stages of the disease.
“You couldn’t study them at the cellular level, so the research field ignored them,” Ozdinler said. She is one of the few scientists in the country who studies cortical motor neurons. Most of ALS research has focused on the death of motor neurons in the spinal cord.
Key Puzzle Piece: Why ALS Moves so Swiftly
But the brain’s motor neurons are a key piece of the ALS puzzle. Their disintegration explains why the disease advances more swiftly than other neurodegenerative diseases. It had previously been thought that the spinal motor neurons died first and their demise led to the secondary death of the brain’s motor neurons. But Ozdinler’s recent research showed that the motor neurons in the brain and spinal cord die simultaneously.
“The whole system collapses at once,” Ozdinler said. “It’s degeneration from both ends, which is why the disease moves so swiftly.”
Every voluntary movement is initiated and modulated by upper motor neurons – answering a cell phone, typing an email, walking to the store. The upper motor neurons tell the spinal motor neurons what to do. In ALS, both the directing neurons and the neurons that create the movement disintegrate at the same time.
Finding the Light that Never Goes Out
Ozdinler spent the last four years figuring out how to permanently sheath cortical motor neurons in fluorescence.
Although scientists can flag spinal cord motor neurons in fluorescence, it wears off as the neuron ages because the process uses an embryonic gene. Ozdinler wanted a longer lasting effect so scientists could study the neuron as it ages and develops ALS. She sorted through 6,000 upper motor neuron genes that are vulnerable to ALS before she found one – UCHL1 – that is expressed through adulthood.
She used that gene – which had been cloned with the fluorescence molecule – and created a mouse model whose upper motor neurons shimmer in green. Then she mated that mouse with an ALS transgenic mouse model. The result is a mouse with fluorescent diseased motor neurons in the brain.
“Now we have a model of one motor neuron population that dies and one that is resistant,” Ozdinler said. “That’s the perfect experiment. You can ask what does this neuron have that makes it resistant and what does the other one have that makes it vulnerable? That’s what we will find out.”
Marina Yasvoina, a graduate student, and Baris Genc, a postdoctoral fellow, both in Ozdinler’s lab, are the lead authors of the paper. Ozdinler collaborated with Gordon Shepherd, MD, PhD, associate professor of physiology, and C.J. Heckman, PhD, professor in physiology, both at Feinberg.
“This work was possible thanks to the collaborative nature of Northwestern,” Ozdinler said.
The research was supported by the Les Turner ALS Foundation, the Wenske Foundation, and the Brain Research Foundation, and grants NS050162, P30 NS054850–01A1, NS061963, and F32 NS063535 from the National Institute of Neurological Disorders and Stroke of the National Institutes of Health and NIH MAD Training Grants 5T32AG020506–09 and 5T32AG020506–10.